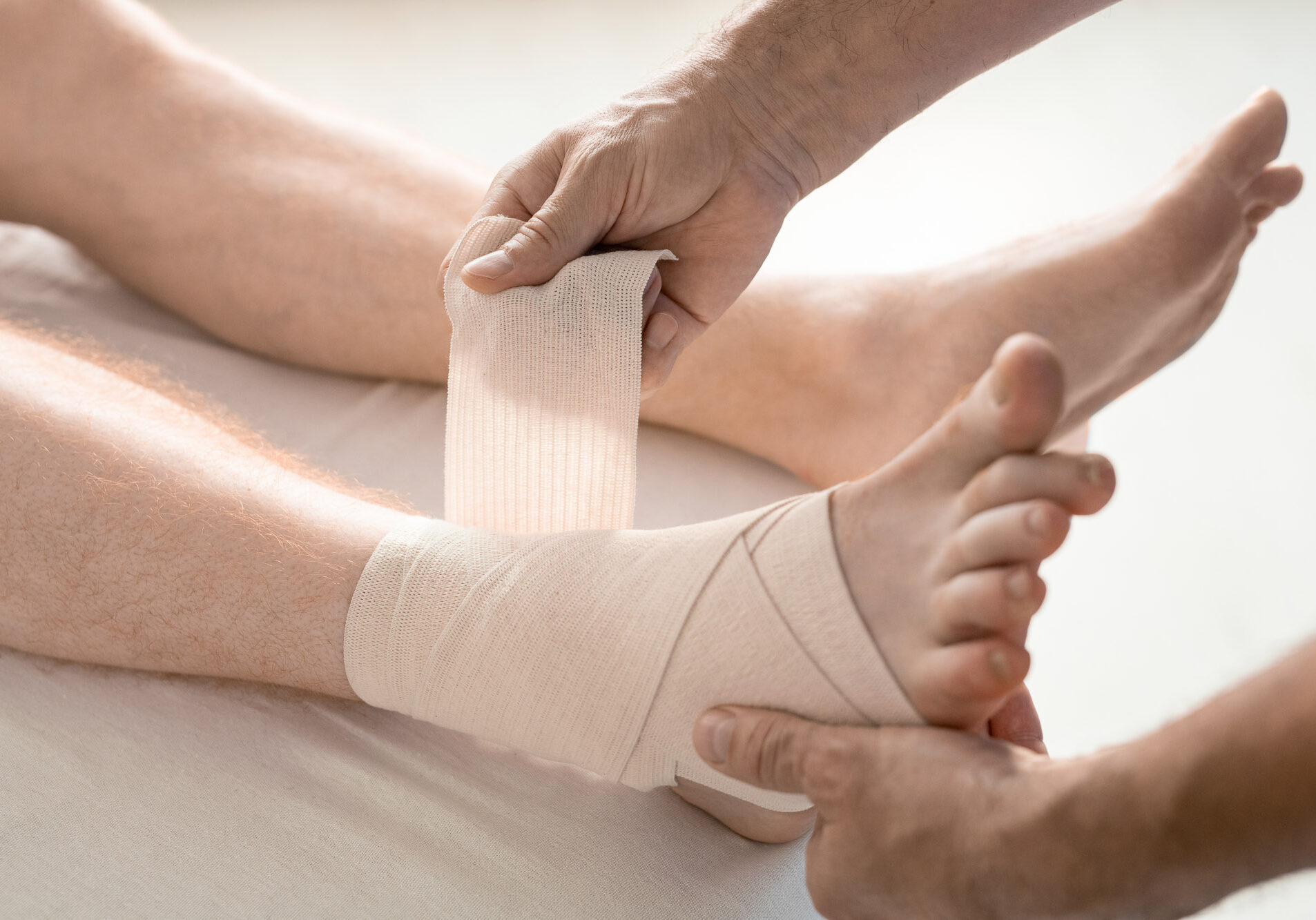
The Achilles Tendon connects the gastrocnemius and calk muscles of the lower leg to the heel. It functions to pull the foot and ankle down during walking and running. An Achilles tendon rupture or tear occurs when the tendon is partially or completely torn due to being overstretched.
Causes
The area of the Achilles that is most frequently torn is near the heal. This area is vulnerable during activities that require lots of direct, forceful jumping and landing. Examples of such activities include basketball and gymnastics. Other potential causes of an Achilles tendon tear include falling and stepping from high to low surfaces (i.e. a hole). Males between the age of 30-40 who participate in recreational sports are most at risk to experience an Achilles tendon rupture.
Symptoms
The first and most noticeable sign of an Achilles tendon tear is a loud popping noise that heard immediately after the rupture. In some cases, the pop is loud enough to be heard by others near the patient. Other common symptoms include the following:
- Pain
- Swelling
- Inability to push off the foot
- Difficulty standing on the toes
Patients who experience the symptoms of an Achilles tendon rupture should make an appointment with an Orthopedic foot and ankle specialist. Diagnosing and treating the injury early is the key to treatment success.
Diagnosis
A physical examination is used to diagnosis an Achilles tendon rupture. During a thorough physical examination, the Orthopedic performs a series of tests to access the severity of the tear. An x-ray may need to be ordered to see if a piece of the heel bone came off during the rupture and an MRI may need to be done to confirm the Orthopedic’s diagnosis.
Treatment
Non-surgical treatment involves the use of a splint or cast. While the tendon is immobilized, it’s torn fibers heal.
Surgical treatment involves the use of sutures and special suturing techniques to repair the tendon and if necessary reattach it to the heel.
Our Specialties
The team at OSNI covers a wide variety of specialties for orthopedic needs. Take a look at them all below and reach out to our team by visiting our contact page to schedule a visit.