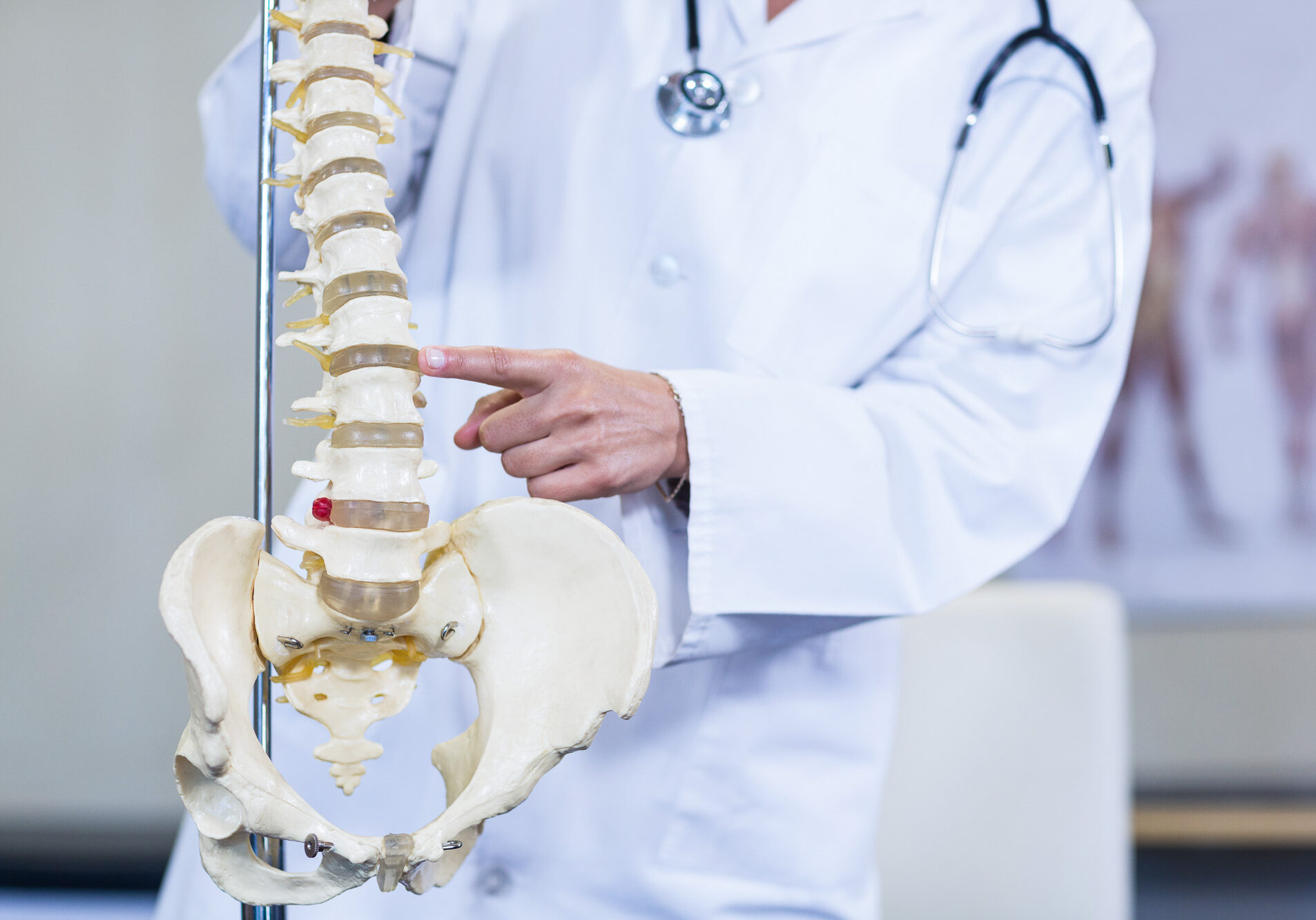
A herniated disc is a common problem that occurs in the lower back and neck. The intervertebral discs that lie between adjacent vertebrae (spinal bones) act as shock absorbers that take pressure off the spine during weight-bearing activities. When the inner portion of the disc protrudes past the outer portion and into the spinal canal, a disc is said to have herniated or slipped. Often times, a herniated disc can pinch a spinal nerve and cause back and/or extremity pain and a host of other unpleasant symptoms.
Causes
A herniated disc can occur when lifting an object without proper form or when lifting an object that is too heavy. It can also occur as a result of the following conditions:
- Degenerative disc disease
- Osteoarthritis of the spine
- Obesity
Smoking and overuse also increase the likelihood of a disc herniating.
Symptoms
The symptoms of a herniated disc may be experienced in the spine or the extremities. They include the following:
- Pain
- Weakness
- Numbness
- Tingling
- Burning
In rare cases, loss of bladder control may occur.
Non-Surgical Treatments
A herniated disc can usually be treated using non-surgical treatment options such as the following:
- Nonsteroidal anti-inflammatory drugs. Medications that reduce pain and swelling.
- Activity modification. Slowing down or stopping activities that are painful.
- Physical therapy. Strengthening and stretching the neck and back muscles help protect and take pressure off the spine.
- Ice. Applying ice to painful areas decreases pain and inflammation.
Patients with a herniated disc should be extra careful when lifting objects and/or bending over as those movements can make the condition worse. Patients who do not get relief from nonsurgical treatments may benefit from a cortisone injection. A quick procedure is performed to inject powerful anti-inflammatory medications into the painful area. If this does not work, the condition may need to be treated using surgical intervention.
Surgical Treatment
A herniated disc may be repaired by removing the part of the disc that is herniated. This is known as a microdiscectomy. A procedure that removes the entire disc and then fuses adjacent vertebrae may also be used. This is known as a microdiscectomy and vertebral fusion. The decision regarding which procedure to perform is based on the severity of the condition and the opinion of the Orthopedic surgeon who is treating it.
Our Specialties
The team at OSNI covers a wide variety of specialties for orthopedic needs. Take a look at them all below and reach out to our team by visiting our contact page to schedule a visit.