Anterior Cruciate Ligament (ACL) injuries are one of the most common types of knee injuries. They are typically sustained by athletes and active individuals who participate in high-impact sports that involving running, jumping, cutting, pivoting, and turning. ACL injuries can vary in severity. Low-level sprains generally heal quickly and do not sideline athletes. Complete tears are serious injuries that usually require surgical intervention and typically sideline athletes for a minimum of 6-8-months.
Causes
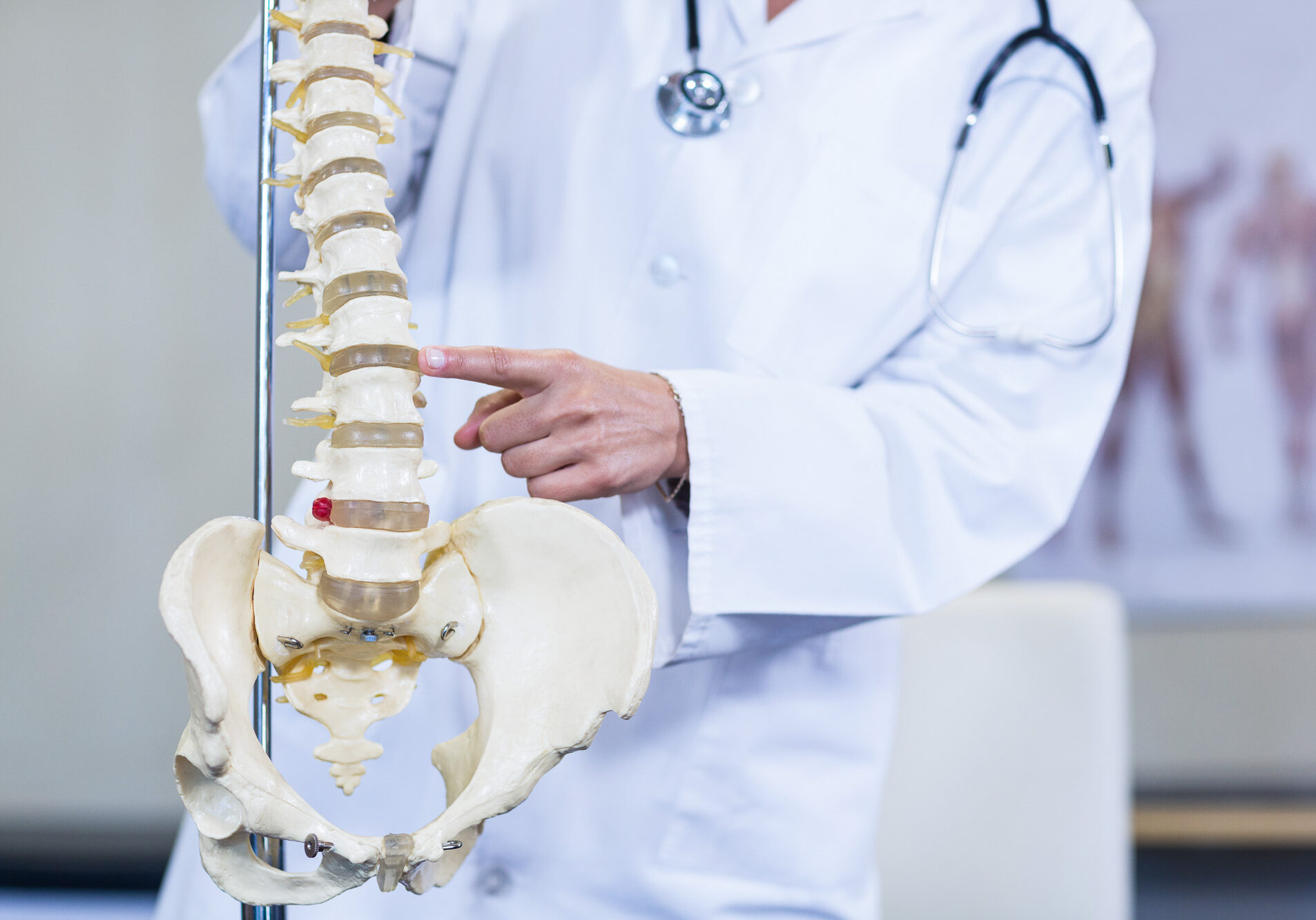
The ACL is one of the cruciate ligaments of the knee. The other cruciate ligament is the posterior cruciate ligament (PCL). The two cross one each other in the knee joint to form an “X”. Both have the important responsibilities of providing back and forth motion of the knee and rotational stability. The PCL is less commonly injured than the ACL. Common causes of ACL injuries include the following:
- Forcefully changing direction
- Suddenly slowing down
- Landing awkwardly while falling
- Direct contact (i.e. a tackle, fall, or blow to the knee)
Symptoms can range in severity depending on the seriousness of the injury. Males are more likely than females to sustain an ACL injury. Athletes who are not in good physical condition are also more likely to sustain ACL injuries.
Symptoms
ACL injuries commonly present with the following symptoms:
- Pain
- Instability
- Decreased range of motion
- Tenderness
Following an ACL injury, patients may have trouble bearing weight on the injured knee. For this reason, crutches are often used after an injury occurs.
Diagnosis
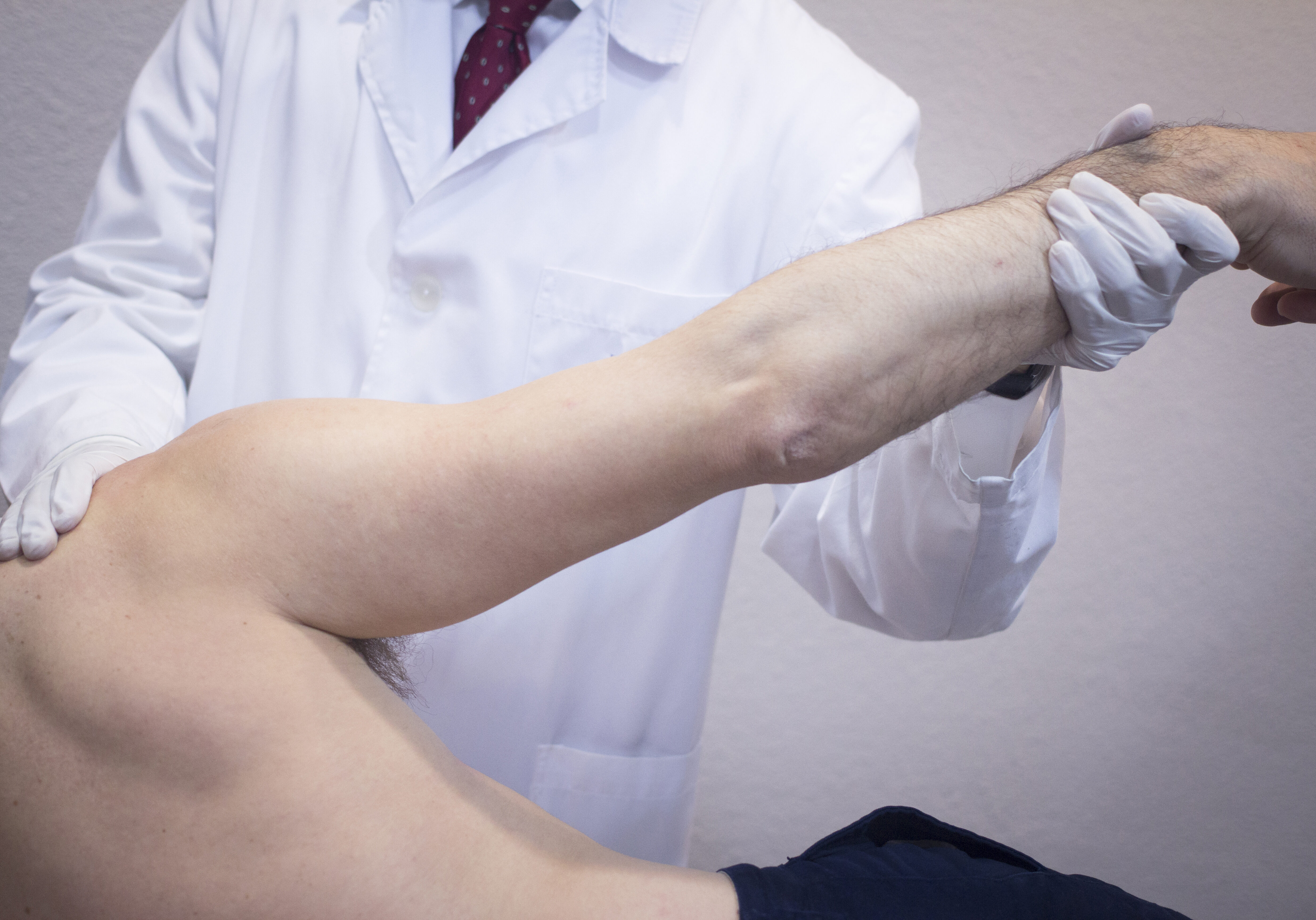
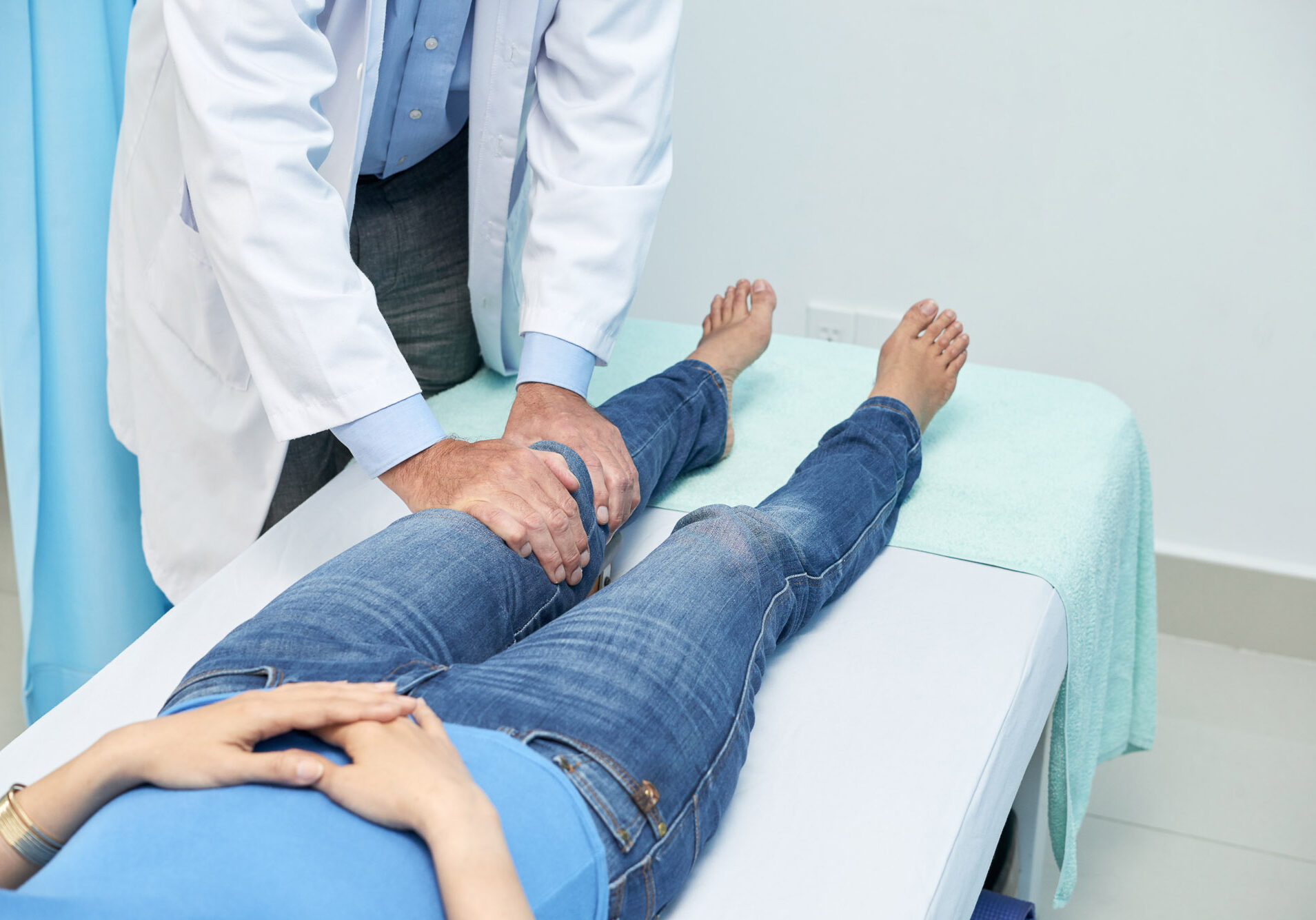
A physical examination, x-ray, and MRI are used to diagnose ACL injuries.
Treatment
Nonsurgical treatment
ACL injuries that do not involve a tear can be treated using the following nonsurgical treatment options:
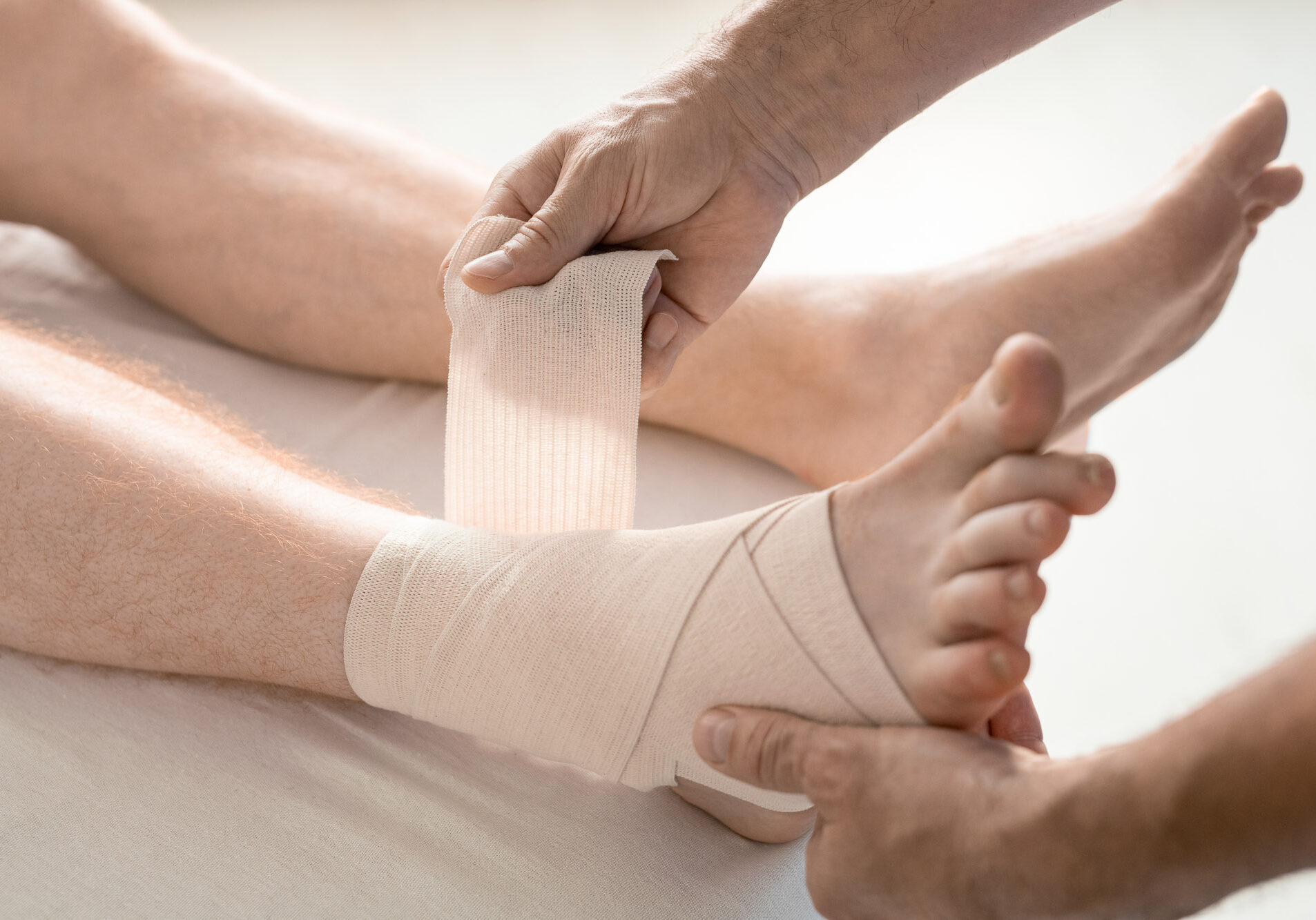
- Rest, Ice, Compression, Elevation (RICE)
- Immobilization (bracing)
- Activity modification
- Anti-inflammatory medications
- Physical therapy
In most cases, a nonsurgical treatment plan will include all these treatment options.
Surgical Treatment
Torn ACLs generally require surgical intervention. An arthroscopic ACL reconstruction is performed. During the procedure, an Orthopedic surgeon replaces the torn ACL with a new one made from an autograft (the patient’s tissue) or an allograft (tissue taken from a cadaver). The procedure takes 1-2-hours. In most cases, patients fully heal 6-8-months after surgery and are allowed to return to competition or activity.
Our Specialties
The team at OSNI covers a wide variety of specialties for orthopedic needs. Take a look at them all below and reach out to our team by visiting our contact page to schedule a visit.